The continual increase in incidence of skin cancer over the past decades is a clear indication of the need for continuing public education on how to reduce the risk of developing skin cancer and awareness of how to detect the early signs.
There are two main types of skin cancer: malignant melanoma which is less common but more serious; and non-melanoma skin cancer, which is very common but not so serious. The commonest non -melanoma skin cancers are basal cell carcinoma and squamous cell carcinoma.
Like most cancers, skin cancer is more common with increasing age, but the incidence of malignant melanoma is disproportionately high in young people with over a third of cases occurring before the age of 55.
If picked up early both non-melanoma and melanoma skin cancers have a good prognosis and even for melanoma 5 year survival rates have risen to around 85% for men and over 90% for women.
Sun exposure is the main cause of skin cancer although there are links of skin cancer to excessive exposure to sun beds. Other factors that influence the risk of skin cancer include people with light eyes or hair, who sunburn easily or do not tan and those with a lot of moles or freckles. Those who have other close family members who have had skin cancer and those who have had previous skin cancers are also more at risk.
It is important to self examine. If one has moles, birthmarks or brown spots look out for changes in colour, an increase in size, a change in texture, irregularity or any itchiness or bleeding. Be aware of any skin growth that increases in size and appears pearly, translucent, tan, brown, black, or multicolored or an open sore that does not heal within three weeks. Self-examination is recommended monthly and if one is concerned one should contact your GP for advice.
Treatments for non-melanoma and melanoma have progressed rapidly over the last decade and it is important to be referred to a specialist once a skin cancer has been diagnosed so that the options can be discussed with you. This may require advice and/or treatment from dermatologists, plastic surgeons, medical and clinical oncologists in order to obtain the best outcomes.
Surgery is often the best way to treat to skin cancer and surgery and reconstruction following skin cancer combines oncological, reconstructive and aesthetic experience to provide the optimal results. Often reconstructive procedures need to be tailored to the individual patient and it is important that for any surgical procedure that the results achievable match the expectations of surgery and the risks and benefits are discussed beforehand.
Basal Cell Carcinomas (BCC’s) or rodent ulcers are the commonest of all cancers in the BCC’s are usually found on sun exposed areas such as the face and neck although can occur all over the body. They are slow growing and are often present for months or years. They do spread around the rest of the body and surgical excision remains the most effective way of removing these common skin tumors.
Squamous Cell Carcinomas (SCC’s) also occur most commonly in sun-exposed areas. Although they are less common than BCC’s they can be more aggressive and occasionally spread to the lymph glands. Like BCC’s surgery remains the most effective means of removing these lesions. For SCC it may be necessary to monitor the lymph node basins either clinically or by the use of ultrasound.
Malignant Melanoma is a cancer of the cells that help to tan the skin. In contrast to BCC and SCC, melanoma can affect younger patients. The main signs are of a mole that is growing, changing shape, changing color, itching and bleeding. It can spread elsewhere around the body and an early detection can lead to improved outcomes. The treatment may involve both surgical removal of the melanoma but also staging of the lymph node basin. Staging may be performed using ultrasound or by an invasive technique called sentinel node biopsy.
Sentinel node biopsy is a technique that can be used (particularly in melanoma) to determine whether there has been any spread to the lymph nodes. It requires a preoperative scan at the time of skin cancer removal and the removal of a lymph node through an incision in the lymph node basin as predicted by the preoperative scan. The lymph node is assessed pathologically and if negative can provide significant reassurance to patients. The pros and cons of the technique need to be weighed up against the risks and complications.
Following a diagnosis of melanoma it is important to keep self examining and maintain regular follow up with regular clinical assessment and surveillance of the lymph node basins which can be provided by ultrasound assessment. This should remain for at least 5 years at regular intervals. Detection of disease at an early stage is paramount in halting the progression of disease. Where spread has occurred further surgery in the form of a lymph node dissection may be necessary. Further treatments such as radiotherapy, chemotherapy and immunotherapy may also need to be considered at this time and you will be advised accordingly.
Reconstruction
Although the most important consideration in the short term is to remove the tumour oncologically in the long term the method of reconstruction is important to provide the optimal reconstructive and aesthetic result. This often can be achieved by closing the defect directly in a straight line to leave a neat scar in an unobtrusive position. Where the lesion or defect is larger a skin grafts or local flaps may be used.
A skin graft is the technique of removing skin from one area of the body and placing it on another. The blood supply to the graft develops over a number of days to weeks. Depending upon what is involved, skin grafts take the form of either full-thickness grafts or split-thickness. Full-thickness Skin Grafts are whole pieces of skin and the site from where the graft is taken is closed directly leaving a scar in this area. They are commonly taken from behind the ear, the neck, the groin and the arm.
Split-thickness skin grafts are usually taken from the thighs and are thin shavings of skin that leave behind them an area similar to a graze. This area heals by itself although can take a number of weeks.
A local flap s a piece of tissue that carries with it its own blood supply. One can utilize an area with excess skin and use it to move it into the area needing to be reconstructed. The area where the flap is taken from is stitched and the resultant scar can be placed in a way that will allow the resultant scar to be less visible.
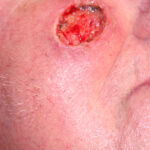

Questions Regarding Skin Cancer
I have had a mole and it has changed colour over the last few weeks and has starting bleeding. What should I do?
When looking at moles and skin lesions one needs to look at the size of the lesion and whether it has changed in size or shape. In terms of shape one should look at whether the lesion is symmetrical or whether there are any irregularities in the lesion i.e. does the lesion have a definite border. It is also important to look at the colour – healthy moles are usually one uniform colour. Usually if your lesion has bled or you have noticed any of the above in your lesion you should have it checked out.
Can Skin Cancer Spread?
The commonest form of skin cancer is Basal Cell Carcinoma in 75% of cases and does not spread. The second commonest form of skin cancer is squamous cell carcinoma (20%) can spread but this is very uncommon (<5%). Although Melanoma is an uncommon form of skin cancer it is the most common form of skin cancer to spread. All patients with melanoma need to be followed up in order to make sure that any signs of spread are picked up as early as possible.
I have had a removal of a basal cell carcinoma and the skin was closed directly. The stitches have been removed and the scar is red. What should I do?
The scar remains quite noticeable for the first 3 to 6 months and then starts getting flatter and paler. Massaging the scar with a moisturising cream two or three times a day for the first few months helps in this process. The scar should be protected from direct exposure to sun during this early period. It is unusual to develop lumpy or irregular scars and usually the scars fade to a pale flat line over the course of 6-12 months. Occasionally the scar may take up to two years to fade.
What Is Basal Cell Carcinoma?
Basal cell carcinoma (BCC) is also known as rodent ulcer. It is the most common type of skin cancer in white-skinned people. It usually occurs on sun-exposed areas of skin in the middle-aged and elderly, but it may grow on any area of skin and can occur in younger people.
I Have A Basal Cell Carcinoma. Do I Need Surgery To Remove It?
Surgery remains the most reliable way to remove basal cell carcinomas and prevent the lesions coming back. There are however many other options including creams (topical chemotherapy), freezing (cryotherapy), curettage (scraping), radiotherapy, and exposure to special light (photodynamic therapy) or laser treatment. The risks and benefits need to be discussed at your consultation.
I Have Had Skin Cancer. Should I Avoid The Sun?
There is no reason to avoid the sun completely. You should protect your skin from ultraviolet radiation in strong sunlight: ideally avoiding exposure to sun between 11am and 4pm and covering up with loose fitting but closely woven clothes. Use a high SPF sunscreen (ideally factor 30 or more) and wear a wide brimmed hat and protective sunglasses.























